We Listen. We Treat. We Care.

Entrust your health and recovery to our dedicated team at Colorectal Practice today.
Get evaluated now
Start a Conversation
Hi! WhatsApp us to enquire now
Our team typically answers quickly.
What Are Piles?
Dr Dennis Koh
Medical Director & Senior Consultant Colorectal Surgeon
MBBS (Nottingham), B Med Sci (Nottingham), MMed (Surgery), FRCS (Edinburgh), FAMS
Dr Sharon Koh
Senior Consultant Colorectal Surgeon
MBBS (Singapore), MMed (Surgery), FRCS (Edinburgh), FAMS
Dr Pauleon Tan
Senior Consultant Colorectal Surgeon
MBBS (Singapore), MMed (Surgery), FRCS (Edinburgh), FAMS

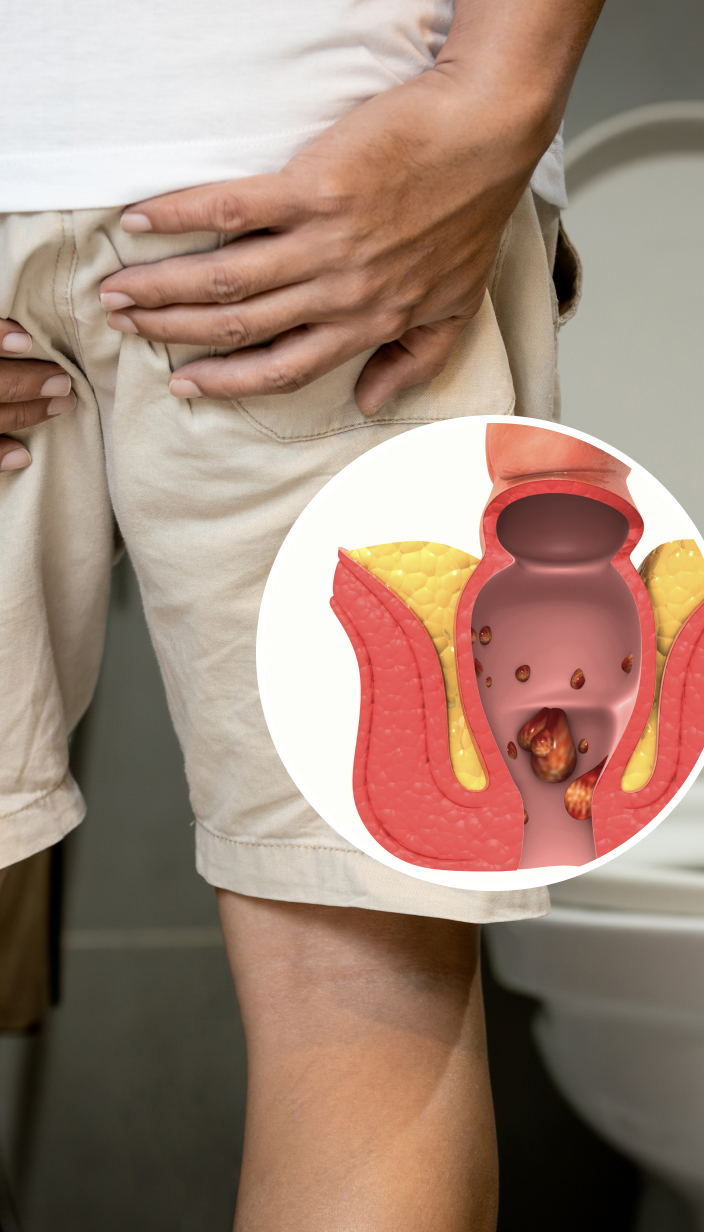
Piles, or haemorrhoids, are enlarged and inflamed blood vessels in and around the anus that are easily traumatized and may bleed during bowel movements.
While mild piles may eventually resolve on their own, moderate to severe piles (if left untreated) may worsen in size and position and may even become strangulated, causing significant pain.

How Do I Know if I Have Piles?
Some common indications of piles are:
- Changes in bowel habits
- Bleeding from the anus during defecation
- Presence of lumps around or at the anus
- Pain during and after bowel movement
- Feeling of itchiness around the anus
Should you experience any of these symptoms, please see a trusted piles surgeon for a detailed assessment.
What Causes Piles?
Piles, or haemorrhoids, can be caused by a plethora of different factors. Some common causes include:
Chronic constipation or diarrhoea
Strong pressure exerted during labour
Prolonged straining during bowel movements

How Are Piles Diagnosed?
Piles are usually diagnosed through a physical examination and a review of your symptoms. In some cases, additional tests may be needed, such as:
Visual Inspection
A colorectal surgeon can detect external haemorrhoids through a visual inspection of the anus and surrounding area.
Digital Rectal Examination (DRE)
By inserting a gloved, lubricated finger into the patient's rectum, a colorectal surgeon can feel for the presence of any abnormalities, such as lumps or swelling.
What Are the Different Types of Piles (Haemorrhoids)?
Piles (Haemorrhoids) can be divided into four types depending on severity:
1st Degree
These are internal piles that bleed during bowel movements, but are not visible with no protrusion on the outside.
2nd Degree
Haemorrhoids bulge out during bowel movements but can retract into the anal canal afterwards, when the straining has stopped.
3rd Degree
Bowel movements have significant bleeding, with large painful piles protruding after each bowel movement. Piles may be manually pushed back into the canal.
4th Degree
These piles cannot be pushed back into the anus and can cause significant pain. Piles in this stage may become strangulated and can only be treated with piles (haemorrhoids) surgery.
What Are Possible Complications of Piles?
If left untreated, piles (haemorrhoids) can result in the following complications:
Anaemia
Haemorrhoid bleeding can lead to anaemia, a red blood cell deficiency caused by insufficient iron due to blood loss. This can cause fatigue, paleness, and shortness of breath.
Thrombosed Haemorrhoid
External haemorrhoids can sometimes develop blood clots, causing severe pain, swelling, inflammation, and the formation of a firm lump near the anus.
Strangulated Haemorrhoid
When the blood supply to an internal haemorrhoid is cut off, it becomes strangulated, which can cause severe pain, tissue damage, and infection.
Infection
In some cases, haemorrhoids can become infected, causing pain, redness, swelling, and pus drainage.
What Are Common Treatments of Piles (Haemorrhoids)?
Different degrees of haemorrhoids require different piles treatments methods. Lower degrees of haemorrhoids may only require lifestyle and dietary changes such as an increase in fibre and fluid intake in order to soften stools, reduce straining and relieve symptoms. However, greater degrees of piles may require you to undergo either a non-surgical treatment or surgical piles treatments such as haemorrhoidectomy, as recommended by your piles surgeon.
Non-Surgical Piles Treatments
1
Oral Medications and Suppositories
These may be prescribed to treat small and/or bleeding piles.
2
Rubber-Band Ligation
A rubber band is placed over the pile to cut off its blood supply, letting it fall off naturally.
3
Energy Ligation of Haemorrhoidal Arteries
This works on the same principle as rubber band ligature, but comes with minimal or no discomfort.
Surgical Piles Treatments (Piles Surgery)
1
Conventional Excisional Haemorrhoidectomy
The prolapsed haemorrhoid is cut off and the wound is left open to heal on its own, there is an uncomfortable recovery process and a long healing time.
2
Closed-wound Excisional Haemorrhoidectomy
This is similar to the conventional method but the wound is stitched shut. This procedure has the shortest recovery time and least amount of pain.
3
Stapled Haemorrhoidectomy
The prolapsed tissue is pulled back to its original position. Afterwards, the cut edges are stapled together for healing.
4
Ligasure Haemorrhoidectomy
Haemorrhoids are cut away using an instrument that removes tissue and stops bleeding simultaneously. This results in minimal blood loss and postoperative pain, with fewer complications compared to conventional haemorrhoidectomy.
The recovery process depends on the type of procedure done. It is normal to experience some flatulence and bleeding during the first 5 to 10 days after the piles surgery. A soft diet will help with smoother passing of stools. To maximise your speed of recovery, your colorectal surgeon will walk you through the recovery process along with any preventive measures you should take. Generally, home-recovery tips are centred around liquid-based and high-fibre diets, warm sitz baths and keeping the affected area clean. You should also remember to gently pat dry the area and not rub as this may irritate the wound.
Can Piles Be Prevented?
While piles cannot be fully prevented, and not all risk factors can be prevented (e.g. pregnancy), there are certain things you can do to lower your risk of developing them:
Eat a High Fibre Diet
Fibre-rich foods such as fruits, vegetables, and whole grains can soften your stool and reduce the time it spends in the colon (colon transit time).
Avoid Straining During Bowel Movements
Straining can significantly increase the pressure within the veins in the lower rectum.
Respond Promptly to Bowel Urges
Use the toilet when needed to avoid constipation and prevent increased pressure on the rectal veins.
Maintain a Healthy Weight
Obesity increases the risk of piles. Adopt a balanced diet and regular exercise to achieve and sustain a healthy body weight.
Exercise Regularly
Engage in exercises like daily half-hour walks to promote healthy bowel function, prevent constipation, and manage weight, reducing the risk and severity of haemorrhoids.
FAQs on Piles (Haemorrhoids)
Showing 1 of 7

Dr Dennis Koh
Medical Director & Senior Consultant Colorectal Surgeon
MBBS (Nottingham), B Med Sci (Nottingham), MMed (Surgery), FRCS (Edinburgh), FAMS
Dr Dennis Koh is a colorectal surgeon specialising in minimally invasive and advanced endoscopic techniques. He trained in Singapore and Switzerland, where he focused on proctology and pelvic floor disorders. A Fellow of the Royal College of Surgeons of Edinburgh and the Academy of Medicine, Singapore, Dr Koh is also passionate about teaching, having served as Assistant Professor at Duke-NUS and Clinical Senior Lecturer at NUS.
About Dr Dennis Koh

Dr Sharon Koh
Senior Consultant Colorectal Surgeon
MBBS (Singapore), MMed (Surgery), FRCS (Edinburgh), FAMS
Dr Sharon Koh is a fellowship-trained colorectal surgeon with expertise in minimally invasive surgery, advanced endoscopy, and inflammatory bowel disease. She trained in advanced colorectal surgery at Cedars-Sinai Medical Center (USA) and Japan. Formerly Director of Endoscopy at Alexandra Health, she also lectures at NUS and is an active member of local and international colorectal societies like the European Society of Coloproctology.
About Dr Sharon Koh

Dr Pauleon Tan
Senior Consultant Colorectal Surgeon
MBBS (Singapore), MMed (Surgery), FRCS (Edinburgh), FAMS
Dr Pauleon Tan is an experienced colorectal surgeon focusing on minimally invasive surgery, advanced endoscopy and cancer care. After receiving the MOH Health Manpower Development Plan award, he trained in Japan, where he mastered advanced techniques to improve cancer outcomes. Dr Tan has held key roles such as Clinical Director of the Colorectal Cancer Screening Programme at KTPH and is dedicated to delivering patient-centred care.
About Dr Pauleon Tan
We Listen. We Treat. We Care.
Entrust your health and recovery to our dedicated team at Colorectal Practice today. From prompt consults to treatment and recovery, we are committed to seeing you through to a better quality of life.
Our Clinics’ Locations
With a comprehensive network of clinics in Singapore, we stand ready to help you achieve optimal colorectal health.











