
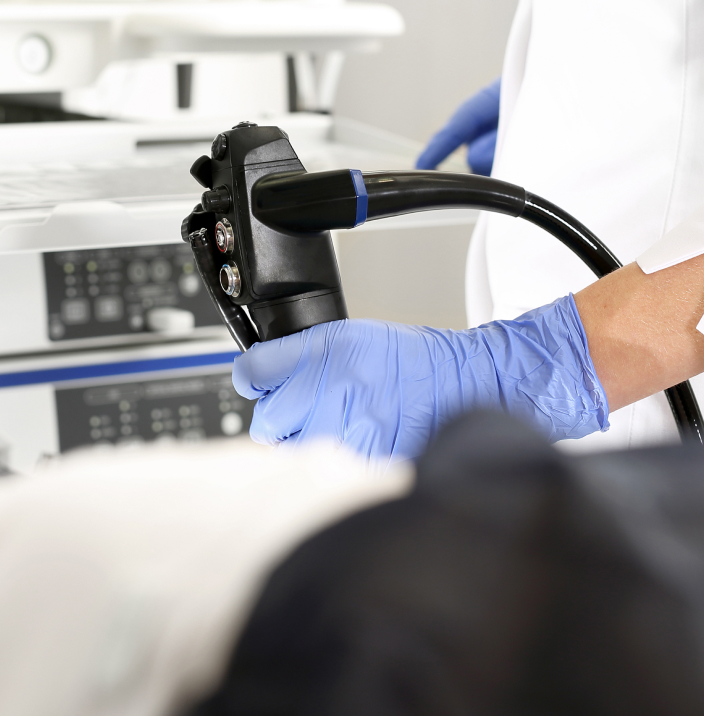
Colonoscopy is a diagnostic procedure that is performed to examine the entire colon and rectum under direct visualisation. By inserting a thin, flexible tube with a small light and camera at the end through the anus and rectum until it reaches the beginning of the colon, we will be able to detect any abnormal growths that may be present in the large intestines.
During this examination, any polyp that is found will be removed to prevent colorectal cancer from potentially developing and a biopsy of the tissues can be carried out for further testing. This is why colonoscopies are known to be highly effective and recommended for diagnosing colorectal cancer at an early stage, which leads to better outcomes for patients.
As colonoscopy is usually done under sedation, it is painless with only minor discomfort such as bloating after the procedure.
When Is a Colonoscopy Recommended?
Who Should Undergo aColonoscopy?
- Obesity
- Excessive cigarette and alcohol use
- High consumption of processed and red meats


How to Prepare for a
Colonoscopy?
A clean bowel is crucial for the clear visualisation of the colon during the procedure. Patients typically follow a liquid diet and use laxatives leading up to the day of the procedure.
Fasting for at least six hours before the procedure ensures an empty stomach which enhances the safety of the procedure, which is performed under anaesthesia.

What to expect during a colonoscopy?
A colonoscopy is an outpatient procedure. This is usually performed under anaesthesia for patient comfort. Typically, a colonoscopy can take about 20–40 minutes to complete. Below is a quick overview of the entire procedure:
- Sedation – To ensure comfort, the patient will receive a sedative or anaesthetic before the procedure.
- Insertion of the Colonoscope – Once the sedation has taken effect, the patient is positioned on their side with knees bent. A colonoscope is then gently inserted through the anus to examine the colon for abnormalities like inflammation, ulcers, or polyps. Air may be pumped into the colon for better visualisation.
- Biopsy and Polyps Removal – If any concerning areas or polyps are detected during the examination, the doctor can perform a biopsy (taking a small tissue sample) or remove the polyps directly using specialised instruments passed through a channel in the colonoscope.
- Completion of the Procedure – After the examination, the colonoscope is removed, and the patient is monitored before being deemed fit for discharge.
What happens after a colonoscopy?
Following the colonoscopy procedure, patients may experience some temporary discomfort, such as gas or bloating, due to residual air in the colon. Additionally, reduced bowel movements in the days following the procedure are common, as the bowel preparation effectively clears a significant amount of stool. It is crucial to rest for the remainder of the procedure day until the effects of sedation fully wear off. During this time, refrain from driving, operating machinery, or making important decisions.
Most patients are able to resume normal activities the day after their colonoscopy. However, seek medical attention if you experience severe bleeding, abdominal pain, dizziness, or fever.
What do the results of my colonoscopy mean?
After the colonoscopy, the doctor will schedule a follow-up appointment to discuss the test results and findings.
Negative Result
A negative outcome from a colonoscopy indicates that no abnormalities were found during the procedure. While this is reassuring, it is important to note that it does not completely eliminate the risk of colorectal cancer. For low-risk individuals, doctors typically recommend future screenings every ten years starting at age 50.
Positive Result
If abnormalities such as polyps or abnormal tissue are found, further evaluation and treatment may be necessary. In many cases, polyps are removed during the colonoscopy itself, and samples are sent to the laboratory for additional testing to determine whether they are cancerous or not. Depending on the results, the doctor may schedule follow-up screenings and recommend treatments, if necessary.
What Are the Risks Involved in Undergoing a Colonoscopy?
The risks involved in colonoscopy are very low, particularly in experienced hands. There are two main risks: bleeding and perforation.
If bleeding occurs, it will typically occur 7–10 days after the procedure. The incidence rate is very low, occurring at about 1–6 in 1000 cases. It is self-limiting and can be treated conservatively.
Perforation during colonoscopy is also very rare, occurring in less than 1 in 1000 cases.
Are There Alternatives to
Undergoing Colonoscopy?
Barium Enema
CT Colonography
A CT Colonography, or virtual colonoscopy, differs from Colonoscopy in that a CT scanner is used to screen for polyps in the large intestine. Here, a tube is inserted into the rectum to inflate the colon with gas while CT images of the colon and rectum are taken from various angles.
While these options also detect the presence of polyps in the colon, they are less accurate than colonoscopy; and should polyps be found, colonoscopy will have to be performed anyway in order to remove them. This is why colonoscopy is usually the most recommended diagnostic method for colon cancer. Nonetheless, we will advise you accordingly based on your needs and preferences.
Flexible Sigmoidoscopy
Flexible sigmoidoscopy is a procedure that examines the rectum and the lower part of the colon, using a shorter, flexible scope. This test is less invasive and requires less extensive bowel preparation. However, it cannot visualise the entire colon and could potentially miss polyps in the upper colon.
While these options also detect the presence of polyps in the colon, they are less accurate than colonoscopy, and if polyps are found, colonoscopy will have to be performed anyway in order to remove them. This is why colonoscopy is usually the most recommended diagnostic method for colon cancer. Nonetheless, we will advise you accordingly based on your needs and preferences.

FAQs on Colonoscopy
References and Other Useful Links














